When to Stop Assessing
Why More Findings Do Not Always Create More Clarity
Assessment is meant to inform action. When it stops doing that, it has stopped being assessment and started being avoidance.
- Updated - May 7, 2026
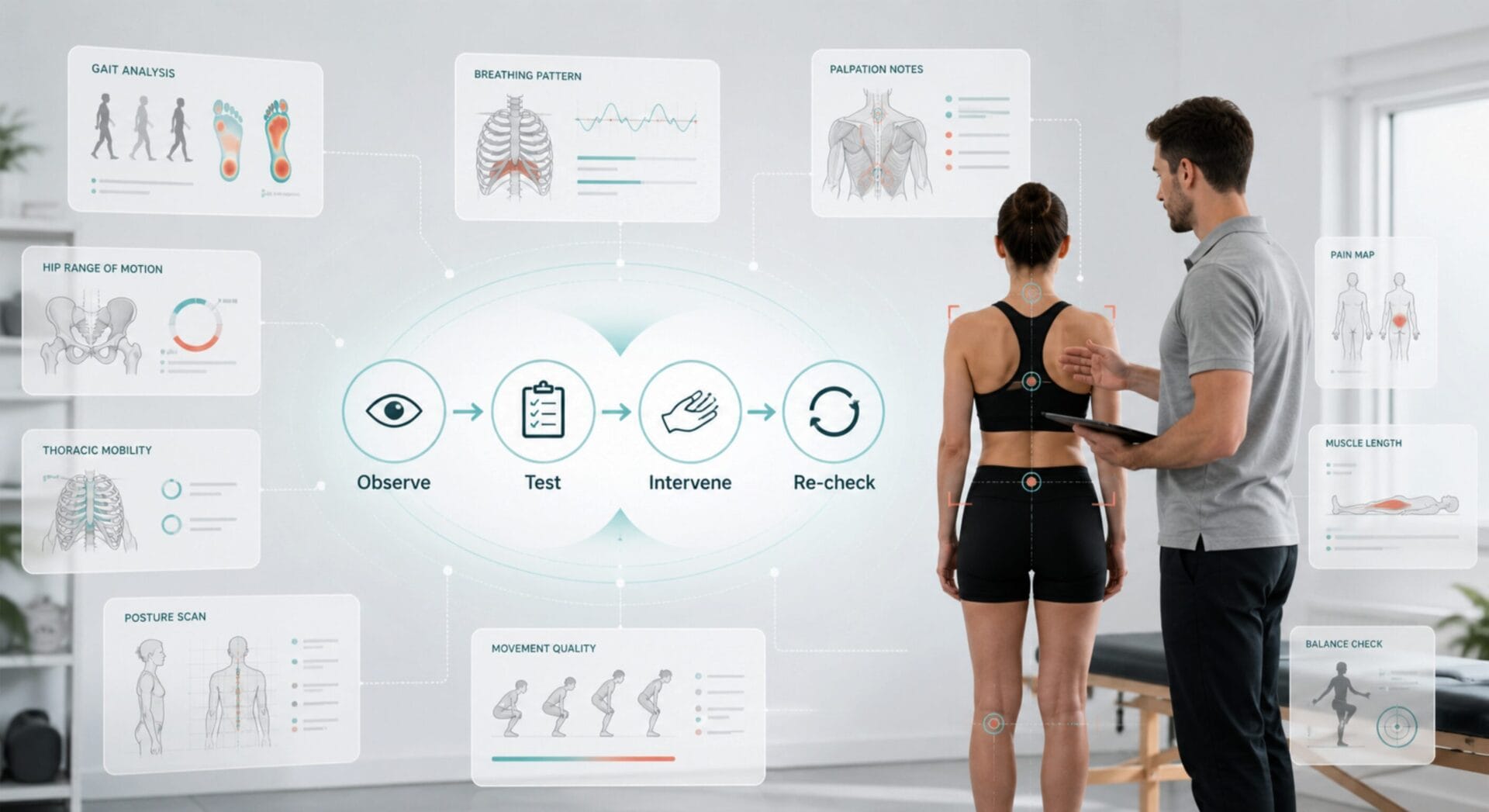
A practitioner has been assessing for twenty-five minutes. They have a structural scan, gait observations, hip range of motion, thoracic mobility, breathing patterns, and palpation findings.
They are still not sure where to start.
The problem is not a lack of information. The problem is too much information without hierarchy.
The Clinical Triangle organises findings into a hierarchy, serving as the reasoning core of Structural Pattern Recognition. It sorts what you have observed into three categories: what is driving the presentation, what is compensating, and what the function demands.
This is one of the most common patterns I see in experienced practitioners. The instinct to keep gathering data feels responsible. It looks thorough. But beyond a certain point, additional findings stop clarifying and start creating noise.
Assessment is meant to inform action. When it stops doing that, it has stopped being assessment and started being avoidance.
A clarification before going further. This essay is about clinical reasoning, not safety screening. Red flag identification, scope-of-practice checks, and contraindication screening are not optional and are not what the Stopping Rule is about. The Stopping Rule is one of three disambiguation rules inside the Clinical Triangle, and it applies to the reasoning layer of assessment, where additional findings begin to compete rather than clarify.
Why This Happens
Most practitioner training rewards thoroughness. Comprehensive assessment is held up as a marker of clinical maturity. Skip a region, and you might miss the cause. Add a test, and you might find the answer.
The assumption underneath this is that the next finding will resolve the uncertainty.
It rarely does.
What the next finding usually does is add another variable to a list that already has too many. The practitioner is not stuck because they need more data. They are stuck because they have not yet built the reasoning structure that turns data into a clinical decision.
This is not a flaw in any modality. Every assessment tradition I know of, whether it comes from physiotherapy, osteopathy, chiropractic, Rolfing Structural Integration, exercise physiology, or movement-based approaches like Feldenkrais and the Alexander Technique, can teach a practitioner to find more than they can interpret.
The skill that resolves this is not more assessment. It is the discipline to stop.
"Verification, not certainty, is what builds clinical confidence."
The Stopping Rule

The Stopping Rule is one of three disambiguation rules I teach inside the Clinical Triangle methodology. It is deceptively simple:
Stop assessing when you have enough information to form a working hypothesis, test it, intervene, and re-check.
That is the threshold. Not certainty. Not a complete picture. Enough to act intelligently and verify the result.
A working hypothesis is not a guess. It has three components:
- A proposed driver. What appears to be organizing the pattern.
- A predicted relationship. How the compensation and function elements follow from that driver.
- A test that can confirm or disconfirm it. A small intervention whose result will be informative regardless of which way it falls.
If you cannot name all three, you do not yet have a working hypothesis. You have a hunch. Hunches are useful, but they are not what the Stopping Rule is asking you to form.
Most practitioners are well past this threshold by the time they realize they have stopped reasoning and started accumulating.
The Reasoning Loop
The Stopping Rule only makes sense inside the broader Reasoning Loop:
Observe → Test → Intervene → Re-check
The loop is the engine of clinical reasoning. Each turn of the loop refines the working hypothesis. The re-check is the most important step because it’s where verification happens.
The first hypothesis is often wrong. That is not a failure of reasoning. The loop is how you find out. A recheck that disconfirms the hypothesis is more informative than another twenty minutes of assessment that never tested it. Being wrong inside the loop produces clinical information. Being uncertain outside the loop does not.
Verification, not certainty, is what builds clinical confidence.
A practitioner who has run the loop three times with the same client knows more about that client’s pattern than a practitioner who has assessed for an hour without acting. The practitioner who acts and re-checks learns something the practitioner who keeps testing cannot.
What This Looks Like in Practice
Consider the same client with low back pain. Two practitioners assess them.
Practitioner A performs a complete structural scan, gait analysis, full range of motion screening of the hip and lumbar spine, thoracic mobility, breathing assessment, palpation, and a movement screen. Forty minutes in, they have eleven findings and no decision about where to start. They keep assessing. The session ends without an intervention.
Practitioner B performs a structural scan, observes the client walk, and palpates the restricted areas. Twelve minutes in, they form a hypothesis: the client’s primary driver appears to be a thoracic restriction limiting rotational capacity, with the lumbar pain as compensation. They test the hypothesis with a brief mobilization of the thoracic segment and recheck the lumbar pain on movement. The pain has reduced. They have learned something.
Practitioner A has more data. Practitioner B has more clinical information.
These are not the same thing.
How to Apply the Stopping Rule
Three questions to ask during any assessment:
- Do I have enough to form a working hypothesis about what is driving this presentation?
- Can I test that hypothesis with a small intervention?
- Will the recheck tell me something I do not already know?
If the answer to all three is yes, stop assessing. Move into the loop.
If the answer to any of them is no, the next assessment step should be chosen specifically to answer that question. Not as a general continuation of the assessment process.
This is the difference between assessment as a sequence and assessment as a strategy.
Signs You May Be Over-Assessing
A few markers that suggest the threshold has already been crossed:
- You have noticed more than you can hold in working memory.
- You are still adding tests, but no longer revising your hypothesis.
- You cannot articulate what would change if you found one more thing.
- You feel busy but not clearer.
- You have not formed a hypothesis at all; you have only listed findings.
If two or more of these are true during a session, the next step is not another assessment. It is to stop, name a working hypothesis, and run the loop.
The Cost of Not Stopping
Practitioners who do not develop the Stopping Rule tend to fall into one of two patterns.
The first is paralysis. They keep assessing, never act, and the session becomes a long observation without intervention. The client leaves with a detailed report of what is wrong, but their experience remains unchanged.
The second is delayed paralysis. They eventually act, but they act late, with too many variables in mind, and without a clear hypothesis. Their interventions feel scattered. The re-check, if it happens at all, cannot tell them which intervention did what.
Both patterns are common. Both are expensive. Both come from the same root: the belief that more information is the cure for uncertainty.
It is not. The cure for uncertainty is the loop.
What to Do Next
If this idea is new to your practice, the next step is small. In your next three client sessions, set yourself the constraint of forming a working hypothesis within fifteen minutes. Test it. Re-check.
You will find that your reasoning sharpens. You will also find that you stop accumulating findings you did not need.
The Clinical Triangle methodology, including the Stopping Rule, the Reasoning Loop, and the disambiguation rules that govern interpretation, is the foundation of Clinical Pattern Recognition Made Simple, a self-paced course for allied health practitioners working with structural and movement presentations.
If you want a shorter introduction to the reasoning model, the Clinical Reasoning Starter Guide is a free download that lays out the framework in eight pages.
The work is not to know more. The work is to know enough, to act, and to verify.
That is what good clinical reasoning looks like.

PLEASE NOTE
PostureGeek.com does not provide medical advice. This information is for educational purposes only and is not intended to be a substitute for professional medical attention. The information provided should not replace the advice and expertise of an accredited health care provider. Any inquiry into your care and any potential impact on your health and wellbeing should be directed to your health care provider. All information is for educational purposes only and is not intended to be a substitute for professional medical care or treatment.
About the author
Join our conversation online and stay updated with our latest articles.
Find Expert Posture Practitioner Near You
Discover our Posture Focused Practitioner Directory, tailored to connect you with local experts committed to Improving Balance, Reducing Pain, and Enhancing Mobility.
