Table of Contents
Understanding Ehlers Danlos Syndrome: A Comprehensive Guide
Ehlers-Danlos Syndrome (EDS) is a complex and often misunderstood group of disorders that affect the connective tissues in the body.
These tissues provide strength and elasticity to the skin, joints, blood vessels, and other vital organs. Due to the wide range of symptoms and the varying severity, EDS can be challenging to diagnose and manage.
This guide aims to shed light on this condition, from its genetic roots to the daily realities faced by those living with EDS.
What is Ehlers Danlos Syndrome?
Definition and Background
Ehlers-Danlos Syndrome encompasses a group of hereditary connective tissue disorders characterized by a variety of symptoms, including but not limited to hypermobile joints, highly elastic skin (stretchy skin), and fragile tissues (skin fragility).
The syndrome is named after Edvard Ehlers and Henri-Alexandre Danlos, who first described the condition in the early 20th century. Despite its long history, EDS remains underrecognized and underdiagnosed.
Types of Ehlers Danlos Syndrome (EDS)

Hypermobile Ehlers Danlos Syndrome (hEDS)
Hypermobile Ehlers Danlos Syndrome is the most common type and is primarily characterized by joint hypermobility, joint pain, and instability. Joint Hypermobility Syndrome symptoms can range from mild to disabling and often include:
- Frequent joint dislocations and subluxations.
- Chronic pain is often described as widespread and persistent.
- Soft, smooth skin that may be slightly more elastic than usual, but not to the extent seen in other types of EDS.
The genetic cause of hEDS is not yet fully understood, and there is currently no definitive genetic test for this type, making diagnosis based on clinical evaluation and family history.
Classical Ehlers Danlos Syndrome (cEDS)
Classical EDS is known for its highly elastic (stretchy) skin and widespread joint hypermobility. Key features include:
- Skin that stretches much more than expected and returns to its original shape slowly.
- Fragile skin that bruises and scars easily; wounds may take longer to heal and leave characteristic “cigarette paper” scars.
- Joint hypermobility leading to frequent dislocations, particularly in the knees, elbows, and shoulders.
Vascular Ehlers Danlos Syndrome (vEDS)
Vascular Ehlers Danlos Syndrome is less common but is considered the most severe form due to its potential life-threatening complications. It is characterized by:
- Thin, translucent skin through which veins can be seen clearly.
- Increased risk of serious complications such as arterial or organ rupture.
- Characteristic facial features, including thin lips, a small chin, and large eyes.
Other Types of Ehlers Danlos Syndrome
In addition to the three main types described above, there are several less common types of EDS, each associated with unique genetic mutations and clinical manifestations:
- Kyphoscoliotic EDS (kEDS): Characterized by severe kyphoscoliosis (outward and sideways curvature of the spine), muscle hypotonia (reduced muscle tone), and fragile sclera (the white outer layer of the eyeball).
- Arthrochalasia EDS (aEDS): Marked by severe joint hypermobility, frequent dislocations, and congenital hip dislocation.
- Dermatosparaxis EDS (dEDS): Features extremely fragile and saggy skin, along with severe bruising and scarring.
- Brittle Cornea Syndrome (BCS): A subtype that primarily affects the eyes, leading to thin corneas and an increased risk of corneal rupture.
Each type has specific diagnostic criteria, and genetic testing plays a crucial role in confirming the diagnosis. Understanding the differences between the types of EDS is essential for providing appropriate care and support to individuals affected by these diverse and challenging disorders.
Causes and Genetics
Genetic Causes and factors
Connective tissues provide structural support to skin, bones, blood vessels, and other organs. In EDS, mutations in specific genes lead to defects in the collagen and connective tissue, resulting in the various symptoms associated with the syndrome. For example:
- Collagen Structure Alterations: Mutations may cause collagen to be structured improperly, making it weaker and less effective at providing necessary support.
- Collagen Production Issues: Some genetic mutations lead to reduced collagen production, resulting in a deficiency that affects the strength and elasticity of connective tissues.
- Processing Defects: Other mutations interfere with the processing and assembly of collagen, preventing the formation of a stable and functional connective tissue matrix.
Specific Genetic Mutations and EDS Types
Each type of EDS is associated with mutations in specific genes, which explains the diversity in symptoms and manifestations among the different types. For instance:
- Hypermobile EDS (hEDS): The genetic cause remains largely unidentified, making it a diagnosis of exclusion. Research is ongoing to pinpoint the underlying genetic factors.
- Classical EDS (cEDS): Typically caused by mutations in the COL5A1 or COL5A2 genes, which are involved in the production of type V collagen.
- Vascular EDS (vEDS): Most often results from mutations in the COL3A1 gene, affecting type III collagen, which is crucial for the integrity of blood vessels and organs.
Inheritance Patterns
EDS can follow different inheritance patterns depending on the type:
- Autosomal Dominant: This is the most common inheritance pattern for EDS, where only one copy of the mutated gene, inherited from an affected parent, is sufficient to cause the disorder. This pattern applies to types like hEDS, cEDS, and vEDS.
- Autosomal Recessive: Some forms of EDS, such as the kyphoscoliotic type, follow this pattern, where an individual must inherit two copies of the mutated gene, one from each parent, to be affected. Parents of an individual with an autosomal recessive type are typically carriers but do not show symptoms of the disorder.
Genetic Testing and Diagnosis
Genetic testing plays a crucial role in diagnosing many types of EDS, especially those with identified genetic mutations. It involves analyzing DNA to identify mutations in specific EDS-related genes. However, diagnosis relies on clinical criteria and family history for types like hEDS, where the genetic markers have not yet been identified.
Environmental and Epigenetic Factors
While genetics play a central role in the development of EDS, environmental factors and epigenetics may also influence the severity and expression of the disorder. Lifestyle choices, physical activity levels, and environmental exposures can impact the health and resilience of connective tissues, potentially affecting the manifestation of symptoms in individuals with EDS.
Understanding the genetic underpinnings and inheritance patterns of EDS not only aids in accurate diagnosis and management but also opens avenues for future research, potentially leading to targeted therapies and interventions for those affected by this complex group of disorders.Symptoms and Diagnosis
Symptoms and Diagnosis
Common Symptoms
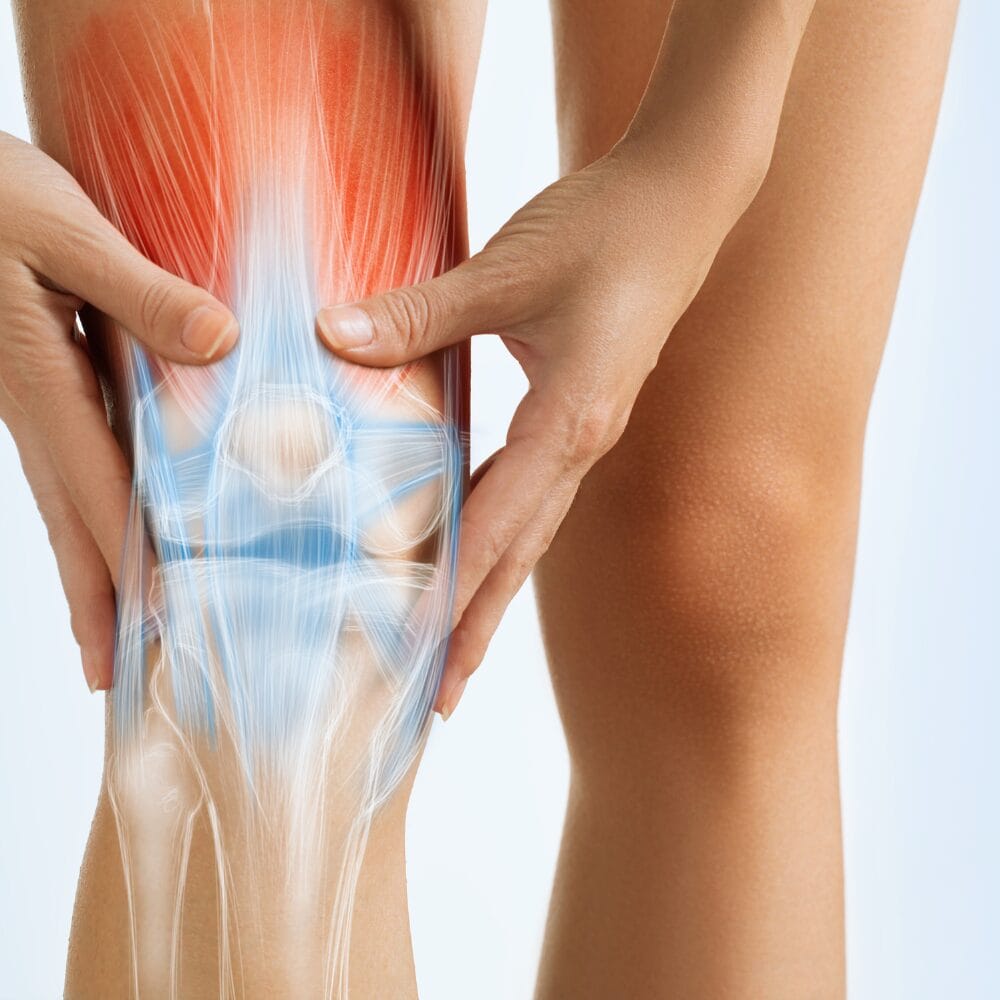
The symptoms of EDS vary widely among individuals and different types of the syndrome, but some commonalities exist, including:
- Joint Hypermobility: This hallmark feature involves joints that stretch farther than expected, leading to a range of issues from pain and instability to frequent dislocations and subluxations. It can affect any joint but is most noticeable in the knees, shoulders, elbows, and fingers.
- Skin Hyperextensibility and Fragility: Many individuals with EDS have soft, velvety skin that stretches more than typical and is fragile, tearing or bruising easily. The skin’s ability to snap back after being stretched can be slow, and wound healing is often delayed, resulting in atypical scarring.
- Vascular Complications: Particularly in vascular EDS, there’s a risk of life-threatening complications such as arterial or organ rupture due to the fragility of blood vessel walls.
- Chronic Pain and Fatigue: Persistent pain, which can be musculoskeletal, neuropathic, or of unknown origin, is a common complaint among individuals with EDS. Fatigue, both physical and mental, significantly impacts daily functioning and quality of life.
- Autonomic Dysregulation: Issues like orthostatic intolerance, temperature regulation problems, and digestive system abnormalities are common, likely due to the involvement of connective tissue in the autonomic nervous system.
- Other Systemic Manifestations: EDS can affect multiple body systems, leading to a diverse array of symptoms, including gastrointestinal issues, dental problems, cardiovascular abnormalities, and more, depending on the type and severity of the disorder.
Diagnosis Process

Diagnosing EDS is challenging due to the overlap of symptoms with other disorders and the variability within EDS types. The process typically involves:
- Medical History and Clinical Examination: A thorough medical history that includes a family history of similar symptoms is crucial. Clinical examination focuses on signs of EDS, such as skin hyperextensibility, joint hypermobility, and a history of dislocations or other related injuries.
- Beighton Score: This is a simple system to quantify joint hypermobility on a 9-point scale, where a higher score indicates greater hypermobility. It’s particularly useful in diagnosing types of EDS where joint hypermobility is a primary symptom.
- Brighton Criteria: For types like hEDS, where there is no definitive genetic test, the Brighton Criteria are used. These criteria consider a combination of major and minor signs, family history, and the exclusion of other disorders that could explain the symptoms.
- Genetic Testing: Genetic testing can confirm a diagnosis for types of EDS with known genetic mutations, such as classical or vascular EDS. This involves analyzing DNA to look for specific mutations associated with EDS.
- Specialist Referrals: Given the systemic nature of EDS, referrals to specialists such as geneticists, cardiologists, gastroenterologists, and others may be necessary to assess related symptoms and rule out other conditions.
Challenges in Diagnosis
The variability of symptoms, even within the same type of EDS, and the commonality of symptoms with other disorders make diagnosis difficult. Misdiagnosis is common, with individuals often receiving several different diagnoses before EDS is considered. Additionally, the lack of awareness and knowledge about EDS among healthcare professionals can further delay an accurate diagnosis.
In summary, diagnosing EDS is a complex process that requires a comprehensive evaluation of symptoms, a detailed patient and family history, and, when available, genetic testing. Awareness and education about EDS are crucial for healthcare professionals to ensure timely and accurate diagnoses, allowing for the implementation of appropriate management strategies and improving the quality of life for those affected by this multifaceted condition.
Living with Ehlers Danlos Syndrome
Living with Ehlers-Danlos Syndrome (EDS) involves navigating a complex array of challenges that extend beyond the medical to impact every aspect of daily life. Individuals with EDS often require a multifaceted approach to manage their symptoms and maintain their quality of life. This section expands on the strategies and adaptations necessary for living with EDS.
Management and Treatment

EDS has no cure, so management focuses on alleviating symptoms, preventing complications, and maintaining the highest possible quality of life. Treatment plans are highly individualized, taking into account the specific type of EDS, the severity of symptoms, and the patient’s overall health and lifestyle.
- Physical Therapy and Rehabilitation: A cornerstone of EDS management, physical therapy aims to strengthen muscles to better support unstable joints, improve proprioception (sense of joint position), and increase overall physical fitness without exacerbating joint issues. It’s essential for physical therapists to be familiar with EDS to avoid treatments that could cause harm, such as high-impact exercises.
- Pain Management: Chronic pain is a pervasive issue for many with EDS. Pain management strategies can include medications, such as NSAIDs or low-dose antidepressants for neuropathic pain, and non-pharmacological approaches like heat therapy, acupuncture, and mindfulness-based stress reduction techniques.
- Bracing and Assistive Devices: For some, braces or orthotic devices can provide necessary joint support, prevent injuries, and reduce pain. Custom orthotics can be especially helpful for foot and ankle instability.
- Diet and Nutrition: Nutritional counseling can help address gastrointestinal issues common in EDS and ensure a balanced diet that supports overall health. Some individuals may benefit from supplements like vitamin C, which is thought to support collagen synthesis and tissue repair, though this should be discussed with a healthcare provider.
- Surgical Interventions: In cases where joint instability leads to severe pain or disability or when there are complications like organ or vascular involvement, surgery may be necessary. Surgical decisions require careful consideration due to the increased risk of complications, such as poor wound healing and tissue fragility.
Lifestyle and Adaptations
Adapting daily activities and lifestyle is crucial for individuals with EDS to manage their symptoms effectively and protect their joints and tissues from further damage.
- Activity Modification: Recognizing and respecting the body’s limits is essential. This might mean modifying exercise routines, taking frequent breaks during activities, and avoiding activities that strain the joints.
- Ergonomic Adjustments: Creating an ergonomic living and working environment can help reduce strain and prevent injuries. This includes ergonomic furniture, supportive bedding, and tools that assist with daily tasks to minimize joint stress.
- Community and Emotional Support: Living with a chronic, often invisible illness can be isolating. Whether online or in-person, support groups can provide a sense of community, shared experience, and valuable information. Mental health support through counseling or therapy can also be beneficial, helping individuals cope with the emotional and psychological challenges of EDS.
- Education and Advocacy: Educating oneself about EDS, staying informed about new research and treatments, and advocating for one’s health needs are crucial aspects of living with the condition. This also includes educating those around you, such as family, friends, and employers, to foster understanding and support.
Challenges of Daily Living
Individuals with EDS often face numerous challenges in their daily lives, from managing chronic pain and fatigue to navigating healthcare systems and advocating for appropriate care. The variability of symptoms and the “invisible” nature of the condition can lead to misunderstanding and stigma, making social interactions and seeking accommodations more difficult.
Living with Ehlers-Danlos Syndrome requires resilience, adaptability, and a proactive approach to health and well-being. By employing a comprehensive management plan, seeking support, and making necessary lifestyle adaptations, individuals with EDS can lead fulfilling lives despite the challenges posed by the condition.
Final Thoughts
Ehlers-Danlos Syndrome, with its myriad types and manifestations, presents a considerable challenge not only to those who live with it but also to the medical community tasked with its diagnosis and management. The variability of symptoms, the overlap with other conditions, and the often invisible nature of its manifestations mean that individuals with EDS frequently navigate a labyrinthine path to diagnosis and effective treatment. This journey is compounded by the current lack of a cure, making symptom management, preventive strategies, and lifestyle adaptations the cornerstones of living with EDS.
The importance of understanding EDS cannot be overstated. Increased awareness among healthcare professionals leads to earlier diagnoses, more effective management plans, and, ultimately, better quality of life for those affected. For individuals with EDS, knowledge empowers self-advocacy, informed decision-making regarding treatment options, and the ability to educate others about the condition, fostering a supportive environment.
Looking ahead, the horizon is not without hope. Advances in genetic research and a growing interest in the intricacies of connective tissue disorders hold promise for breakthroughs in the understanding and treatment of EDS.
Living with EDS is undeniably challenging, marked by a continuous cycle of adaptation and resilience. Yet, within this journey lies the potential for profound personal growth, community building, and contributions to the broader understanding of human health and resilience. As research advances and awareness grows, the future for those affected by Ehlers-Danlos Syndrome looks increasingly brighter, bolstered by the collective efforts of individuals, families, healthcare professionals, and researchers alike.
In conclusion, while Ehlers-Danlos Syndrome remains a complex and often daunting condition, the path forward is paved with education, support, and the relentless pursuit of knowledge. By embracing these pillars, the EDS community and its allies can continue to make significant strides toward improved care, understanding, and, hopefully, solutions that will ease the burdens of those touched by this multifaceted syndrome.
Research
- Research on Ehlers-Danlos Syndromes (EDS) covers a wide range of topics due to the complexity and heterogeneity of the condition. A comprehensive review published in 2020 highlights that EDS represents a group of hereditary disorders of connective tissue characterized by features like joint hypermobility, soft and hyperextensible skin, abnormal wound healing, and easy bruising. The review identifies fourteen different types of EDS, with known molecular causes for thirteen of these types. These causes are related to variants in 20 different genes, most of which are involved in encoding fibrillar collagen types or enzymes that modify these proteins or glycosaminoglycan chains of proteoglycans. Management of EDS is multifaceted, involving surveillance for major and organ-specific complications and integrated physical and rehabilitative medicine, although specific medical or genetic therapies are not currently available for any type of EDS https://pubmed.ncbi.nlm.nih.gov/32732924/
- Another aspect of EDS research focuses on treatment options, particularly for pain management, which is a significant challenge due to the multifaceted nature of the disease. A retrospective cohort study aimed to investigate the efficacy of various treatment modalities for pain and symptom relief in EDS patients. This study found that complimentary/alternative treatments and occupational therapy, along with bracing, were among the most effective options, with a notable percentage of patients reporting improvement. However, neuropathic modulators were less well tolerated, with a significant proportion of patients experiencing adverse effects. The study underscores the variability in treatment effectiveness and the need for a personalized approach, highlighting the importance of further research to develop a comprehensive treatment database. https://pubmed.ncbi.nlm.nih.gov/32709178/
PLEASE NOTE
PostureGeek.com does not provide medical advice. This information is for educational purposes only and is not intended to be a substitute for professional medical attention. The information provided should not replace the advice and expertise of an accredited health care provider. Any inquiry into your care and any potential impact on your health and wellbeing should be directed to your health care provider. All information is for educational purposes only and is not intended to be a substitute for professional medical care or treatment.
