What Is Lordosis?
- Updated - February 26, 2025
What you need to know
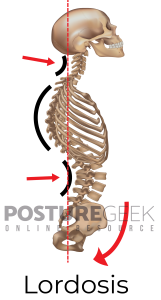
The Spine naturally curves in the neck, torso, and lower back to support bodily functions and maintain balance. Lordosis refers to an excessive inward curve of the Spine, particularly prevalent in the lumbar (lower back) and cervical (neck) regions.
This condition often manifests as an exaggerated arch in the lower back, resembling a “C” shape when viewed from the side, and may be accompanied by a forward head posture in the neck.
Lordosis can significantly impact posture and comfort, commonly arising from a combination of tight muscles, weakened core strength, spinal anomalies, or injuries. It is also closely associated with Lower Cross Syndrome, where imbalanced muscle strength and tightness contribute to the characteristic posture of Lordosis.
In children, a common form of this condition is benign juvenile lordosis, which typically results from weak or tightened muscles around the hips and often corrects itself as the child grows.
By addressing the key features of Lordosis and its common sites, this introduction sets the stage for a deeper exploration of its causes, symptoms, and treatment options.
So, what is lordosis of the lumbar and cervical spine?
- Lumbar Spine: The Lumbar Spine, commonly referred to as the lower back, is the part of the Spine that curves inward near the abdomen. It comprises five vertebrae and is responsible for bearing much of the body’s weight and providing flexibility and movement. Excessive Lumbar lordosis often affects this area, leading to an exaggerated inward curve.
- Cervical Spine: The Cervical Spine refers to the neck portion of the Spine, comprising seven vertebrae that support the head and allow for a wide range of head movements. As the name suggests, Cervical Lordosis in the cervical spine can manifest as an excessive inward curve, often associated with a forward head posture. This condition can strain neck muscles and lead to discomfort.
Understanding the Biomechanics of Lordosis
Lordosis is characterized by an excessive inward curve of the Spine, particularly noticeable in the lumbar (lower back) and cervical (neck) regions. This condition can arise from a complex interplay of muscular imbalances, skeletal alignment, and lifestyle factors. Understanding the biomechanics behind Lordosis is essential to grasp how certain conditions lead to its development. Certain groups are more susceptible to lordosis due to injury, health conditions, and the spine’s compensation for existing imbalances.
Muscular Imbalances and Weak Abdominal Muscles
- Tight Hip Flexors: The hip flexors are muscles at the front of the hips that, when tight, pull the pelvis forward into an anterior tilt. This tilt increases the curvature of the lower back, leading to an exaggerated lumbar lordosis. Tight hip flexors are often a result of prolonged sitting or sedentary lifestyles. While a slight forward curve in the lumbar and cervical regions is natural and helps with shock absorption, an exaggerated curve can lead to posture issues and discomfort.
- Weak Abdominal Muscles: The abdominal muscles, particularly the transversus abdominis and the rectus abdominis, play a crucial role in supporting the Spine and maintaining pelvic alignment. When these muscles are weak, they fail to counteract the forward pull of tight hip flexors, contributing to the forward tilt of the pelvis and deepening the lumbar curve.
Spinal Problems
- Intervertebral Disc Degeneration: Degeneration of the discs between the vertebrae, particularly in the lumbar region, can lead to disc height and flexibility loss. This degeneration can alter the normal curvature of the Spine, contributing to the development of Lordosis.
- Spondylolisthesis occurs when one vertebra slips forward over the one below it, often leading to an exaggerated curvature in the lumbar region as the Spine tries to stabilize itself.
Lifestyle Factors
- Prolonged Sitting: Extended periods of sitting, especially with poor posture, can lead to tightness in the hip flexors and weakening of the abdominal muscles, contributing to the development of Lordosis.
- Lack of Exercise: Insufficient physical activity can lead to weak core muscles, which are crucial for supporting the Spine and maintaining proper posture. The Spine is more susceptible to developing an exaggerated lordotic curve without strong core muscles.
The biomechanics of Lordosis involve a complex interplay of muscular imbalances and structural changes in how the Spine curves. Tight hip flexors and weak abdominal muscles can lead to an anterior pelvic tilt, exacerbating the lumbar curve. Additionally, spinal problems like disc degeneration and spondylolisthesis can contribute to the condition. Understanding these biomechanical relationships is crucial for addressing the root causes of Lordosis and developing effective treatment strategies.
Discover a practitioner near you.
Looking for a practitioner near you? Our extensive network of qualified professionals is here to help you.
Why Can Lordosis Be A Problem?

Immediate and Visible Symptoms
Noticeable Arch in the Lower Back: One of the most apparent signs of Lordosis is an exaggerated inward curve of the lumbar Spine. This can often be observed when looking at the side profile of an individual, where the lower back region curves significantly inward towards the abdomen.
Protruding Abdomen: Due to the exaggerated curvature of the lumbar Spine, the abdomen may protrude more than usual, altering the individual’s posture and potentially affecting balance.
Forward Tilt of the Pelvis: In cases of Lordosis, the pelvis may tilt forward, accentuating the curvature of the lower back. This tilt can sometimes be noticeable when viewing the person from the side.
Gap Between the Lower Back and the Floor: When lying flat on the back, there might be a noticeable gap between the lower back and the floor due to the inward curvature of the Spine.
Long-Term Effects and Symptoms
Chronic Back Pain: Over time, the stress and strain on the Spine and surrounding muscles can lead to persistent lower back pain. This pain may exacerbate after prolonged periods of standing or sitting and might not easily subside with standard pain relief methods.
Reduced Flexibility: The exaggerated curvature can lead to stiffness and decreased flexibility in the lower back, making it difficult to bend or twist the torso. This stiffness can extend to the hips and hamstrings, further limiting mobility.
Muscle Fatigue and Strain: The muscles in the lower back and abdomen may become overworked as they attempt to compensate for the abnormal spinal curvature, leading to muscle fatigue, spasms, and strain.
Impaired Posture and Balance: Long-term Lordosis can affect overall posture, leading to an imbalance that impacts daily activities. Individuals may find maintaining a neutral spine position challenging, affecting how they walk, sit, and engage in physical activities.
Neurological Symptoms: In severe cases, the spinal curvature can compress nerve roots, leading to neurological symptoms such as tingling, numbness, or weakness in the lower extremities.
Impact on Internal Organs: Extreme curvature can eventually impact the positioning and function of internal organs, potentially leading to issues with digestion, respiration, and circulation due to the altered intra-abdominal pressure.
Understanding the full spectrum of Lordosis symptoms, from the immediately visible signs to the long-term health implications, is crucial for early detection and intervention. Recognizing these symptoms can prompt individuals to seek professional assessment and treatment, mitigating the progression and impact of Lordosis on their overall health and quality of life. Addressing Lordosis proactively can help prevent the onset of more severe complications, emphasizing the importance of awareness and education on this condition.
Addressing Lordosis
Physical Therapy Techniques
Manual Therapy: Physical therapists may employ hands-on techniques to manipulate and mobilize the Spine and surrounding tissues. This can help reduce pain, increase range of motion, and improve flexibility in the affected areas.
Postural Training: Therapists can guide patients through exercises and strategies to correct postural habits contributing to Lordosis. This includes training on how to stand, sit, and move in ways that promote a healthier spinal alignment.
Therapeutic Exercises: Specific exercises are designed to strengthen weak muscles and stretch tight muscles, contributing to Lordosis. A balanced approach ensures that the body’s musculature supports the Spine correctly.
Targeted Exercises
Core Strengthening: Exercises like planks, bird dogs, and pelvic tilts strengthen the core muscles, which are crucial for supporting the Spine. A strong core helps maintain proper posture and reduces the strain on the lumbar Spine.
Hip Flexor Stretches: Since tight hip flexors can exacerbate Lordosis, incorporating stretches for these muscles can help reduce the forward tilt of the pelvis. Lunges and kneeling hip flexor stretches are effective options.
Hamstring Stretches: Tight hamstrings can also contribute to Lordosis by pulling down on the pelvis. Incorporating hamstring stretches can help alleviate this tension, promoting better pelvic alignment.
Back Extensions: Gentle back extension exercises can help strengthen the muscles along the spine, improve stability, and reduce the excessive inward lordotic curve associated with Lordosis.
Posture Correction Strategies
Ergonomic Adjustments: Changing the work and living environments to support proper posture can significantly impact managing Lordosis. This includes ergonomic chairs, standing desks, and adequate positioning of screens and keyboards.
Mindful Movement: Being conscious of how one moves throughout the day can help in correcting Lordosis over time. This involves maintaining a neutral pelvis and engaging the core during activities.
Yoga and Pilates: Both disciplines emphasize core strength, flexibility, and mindful movement, making them beneficial for individuals with Lordosis. Specific poses and exercises can be tailored to address the condition’s unique challenges.
Treating any issues that may arise from excessive Lordosis effectively requires a multifaceted approach that combines physical therapy, targeted exercises, and posture correction strategies. Individuals can significantly improve their symptoms and quality of life by strengthening key muscle groups, improving flexibility, and making ergonomic and lifestyle adjustments. Working with healthcare professionals to tailor the treatment plan to the individual’s needs is essential to ensuring the best possible outcomes.
The Role of Professional Diagnosis
Accurate Assessment: Healthcare professionals use a combination of physical examinations, medical history, and imaging tests (like X-rays and MRIs) to diagnose lordosis accurately and determine its extent and severity. A comprehensive physical exam is crucial for observing the patient’s posture and conducting specific movements to assess the curvature of the spine. This thorough evaluation ensures that the treatment addresses the specific needs of the individual.
Differentiating Conditions: Lordosis can be symptomatic of or associated with other spinal conditions, such as scoliosis or kyphosis (often found in the Thoracic Spine). Professionals can distinguish between these conditions and identify underlying causes, ensuring a comprehensive treatment plan.
The Importance of Professional Treatment
Tailored Treatment Plans: Based on the diagnosis, healthcare providers can develop a treatment plan tailored to the individual’s condition, lifestyle, and overall health. This personalized approach increases the effectiveness of the treatment and reduces the risk of further complications. Lordosis treated by healthcare providers often involves close monitoring, especially during growth spurts, and may vary depending on associated conditions and individual factors like age and curve severity.
Safe and Effective Techniques: Professionals are trained to use safe and effective treatment techniques, minimizing the risk of injury or worsening of the condition. They can monitor progress and adjust the treatment as necessary, ensuring optimal outcomes.
Holistic Care: Healthcare providers can offer a holistic approach to treatment, addressing not only the physical aspects of Lordosis but also providing guidance on lifestyle adjustments, ergonomic improvements, and preventive measures to avoid recurrence.
The Risks of Self-Diagnosis and Treatment
Misdiagnosis: Without professional expertise, individuals may misinterpret their symptoms and potentially confuse Lordosis with other conditions, leading to inappropriate treatment strategies.
Ineffective or Harmful Treatments: Self-treatment without proper guidance can cause harm or counterproductive outcomes. Specific exercises or treatments may exacerbate the condition if not performed correctly.
Overlooking Underlying Causes: Self-diagnosis may overlook underlying causes of Lordosis, such as structural abnormalities or other health issues, which can lead to incomplete treatment and persistent symptoms.
Seeking professional advice for diagnosing and treating severe Lordosis is essential to ensure safe, effective, and personalized care. Professional guidance helps accurately diagnose and effectively treat Lordosis and provides comprehensive support for managing the condition and preventing future complications.
Individuals are strongly encouraged to consult healthcare professionals rather than relying on self-diagnosis and treatment, which can lead to suboptimal outcomes and increased risks.
Final Thoughts
Understanding why Lordosis poses a problem is crucial, as its excessive curvature can lead to persistent pain, mobility issues, and further complications if left unaddressed. This underscores the importance of early detection, accurate diagnosis, and a comprehensive treatment approach that includes physical therapy, targeted exercises, and posture correction strategies, all tailored to the individual’s specific needs.
As we conclude, the key takeaway is the importance of taking proactive steps towards understanding and managing Lordosis. Whether you’re experiencing symptoms or are at risk, consulting with healthcare professionals can provide the guidance needed to navigate treatment options effectively. By adopting a proactive approach to health and posture, individuals can mitigate the effects of Lordosis, improve their well-being, and lead a more comfortable, active life.
Remember, knowledge is the first step toward positive change. Empower yourself with information, seek professional advice, and take active steps towards a healthier spine and a better quality of life.
Resources
Articles:
Biomechanics and Posture
- Evaluation of lumbar lordosis in symptomatic individuals and comparative analysis of six different techniques: a retrospective radiologic study.
- Recent research underscores the significance of spinopelvic parameters, such as lumbar lordosis, pelvic incidence, and sacral slope, in maintaining proper spinal alignment. These factors are crucial for understanding how lordosis impacts posture and overall spinal mechanics. By analyzing these parameters, healthcare providers can better tailor interventions to restore natural spinal curvature, which is essential for reducing discomfort and preventing long-term complications associated with lordosis.
About the author
PLEASE NOTE
PostureGeek.com does not provide medical advice. This information is for educational purposes only and is not intended to be a substitute for professional medical attention. The information provided should not replace the advice and expertise of an accredited health care provider. Any inquiry into your care and any potential impact on your health and wellbeing should be directed to your health care provider. All information is for educational purposes only and is not intended to be a substitute for professional medical care or treatment.
FURTHER CONSIDERATIONS
Find Expert Posture Practitioner Near You
Discover our Posture Focused Practitioner Directory, tailored to connect you with local experts committed to Improving Balance, Reducing Pain, and Enhancing Mobility.
